Answering Common Questions About Herd Immunity and Vaccination

COVID-19 vaccines have been readily available to many U.S. adults since spring 2021. But despite consistent messaging from public health experts urging Americans to get the vaccine, and signs on vaccination centers offering walk-in appointments, participation rates remained relatively low. As of Jan. 25, 2022, 63.4% of the U.S. population was fully vaccinated against COVID-19, and 39.9% had also received a booster shot, according to the U.S. Centers for Disease Control and Prevention’s COVID Data Tracker. The World Health Organization (WHO) wants each country to vaccinate at least 70% of its population by mid-2022.
Hesitancy around vaccines is not limited to COVID-19: About half of U.S. adults were vaccinated against the flu for the 2020–2021 season, and participation rates were as low as 41.5% in some states, the CDC reported.
A variety of concerns can prompt hesitancy about getting a vaccine, including the perception that the shot was not effective if an individual later feels under the weather. However, those who receive vaccinations also contribute to a broader public health benefit: herd immunity.
“[People who get their flu shot] are also protecting people who are vulnerable and have poor immune systems from getting that flu,” explained Kelly A. Thompson-Brazill, DNP, ACNP-BC, CCRN-CSC, FCCM, director of the Adult-Gerontology Acute Care Program at the Georgetown University School of Nursing. “And that’s really the big concept of herd immunity. It’s not always just to protect yourself. It’s also, really, to protect the vulnerable people within your community.”
Nursing@Georgetown created this resource to help people learn more about herd immunity by addressing misconceptions and encouraging conversations about the importance of vaccination.
Table of Contents:
What Is Herd Immunity?
Also referred to as “community immunity,” herd immunity is a public health term used to describe a case in which the potential for person-to-person spread is significantly reduced due to the broader community’s resistance against a particular pathogen.
Glossary of Additional Terms
- Active immunity: Immunity as a result of the body’s antibody creation after exposure to disease-causing pathogens, either through natural infection or vaccination.
- Herd immunity threshold: Also called the “critical vaccination level,” this is the approximate percentage of a population that needs to be vaccinated in order to reach herd immunity status.
- Immunity: Resistance to a particular pathogen, or disease-causing bacteria, through antibodies.
- Inactivated vaccine: A vaccine using a killed form of the disease-causing germ. This vaccine usually requires multiple doses over time to form immunity. Examples include the DPT and Hepatitis A vaccines and the flu shot.
- Live attenuated vaccine: A vaccine using a weakened form of a germ to produce an asymptomatic infection and generate an immune response similar to a natural infection, without sickness. Examples include the MMR and chickenpox vaccines.
- Messenger RNA (mRNA) vaccine: A vaccine that teaches cells how to make a protein or a piece of a protein that triggers an immune response in the body and produce antibodies, which provide protection if a person encounters the real pathogen. Examples include the Pfizer-BioNTech and Moderna COVID-19 vaccines.
- Natural infection: Contraction of a disease through person-to-person transmission or interaction with disease-causing bacteria.
- Passive immunity: Immunity after receiving disease-fighting antibodies from an external source.
- R0: (Pronounced “r-naught”) The reproductive number of a disease that describes the average number of additional cases a single infected person creates.
- Subunit vaccine: A vaccine using a component of the germ (such as a specific protein) to produce an immune response. This vaccine does not contain a live germ. Examples include the shingles and HPV vaccines.
- Vaccine: A controlled simulation of natural infection meant to trigger antibody creation that helps fight against the disease later, without sickness.
Why Is Herd Immunity Important?
When enough community members are immune to a virus so that it inhibits spread, even those who are not vaccinated will be protected. The “herd” collectively provides insulated safety to all members, which is important for those who are too high-risk for certain vaccinations.
For example, the yellow fever vaccine should not be administered to individuals who are pregnant, have a weakened immune system, or have specific allergies, according to the CDC guidelines on who should not be vaccinated.
For these individuals, it is important that their community has built an immune response to the yellow fever so they are not at risk of infection and transmission. Individuals who are too high-risk to get a vaccination are often more likely to contract the illness and experience serious symptoms.
Additional barriers to vaccination administration may include:
- Age
- Allergies
- Pregnancy
- Recent blood transfusion
- Underlying medical conditions like lung or heart disease
- Weakened immune system
Elke Jones Zschaebitz, DNP, ARPN, FNP-BC, and faculty member at Georgetown University School of Nursing, likens herd immunity to a perimeter fence that ensures the safety of the broader community.
“It’s like a little nuclear circle,” she said. “So that our babies that can’t get vaccinated yet, or our pregnant mothers, or our elderly with immune systems [that] are not as robust, or people who have certain kinds of conditions that they don’t have the correct immunity, will have protection from the active pathogen that could possibly harm or kill them.”
The Science Behind How Herd Immunity Works
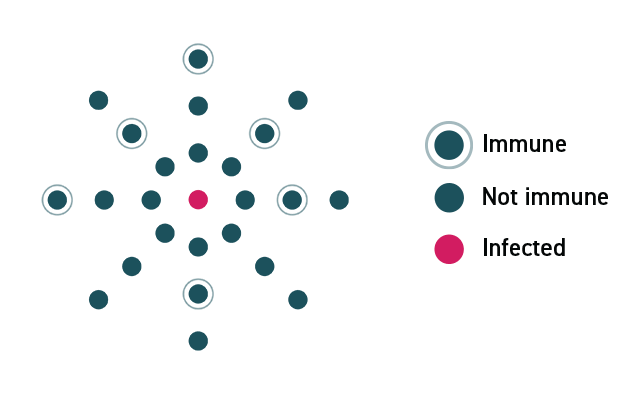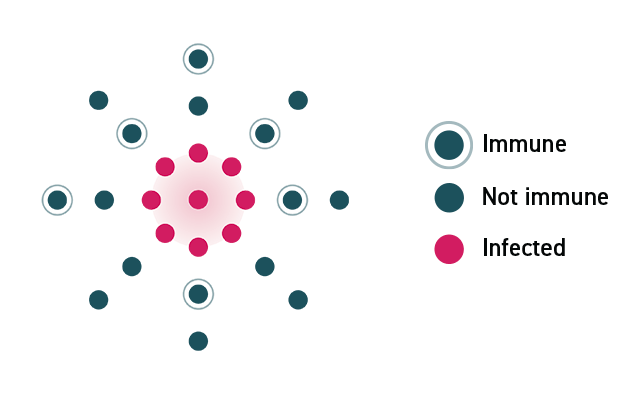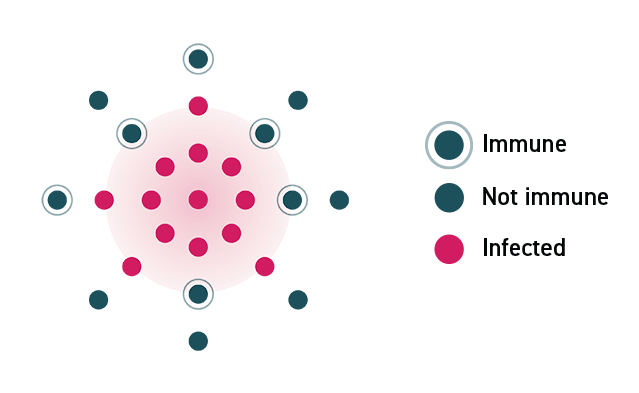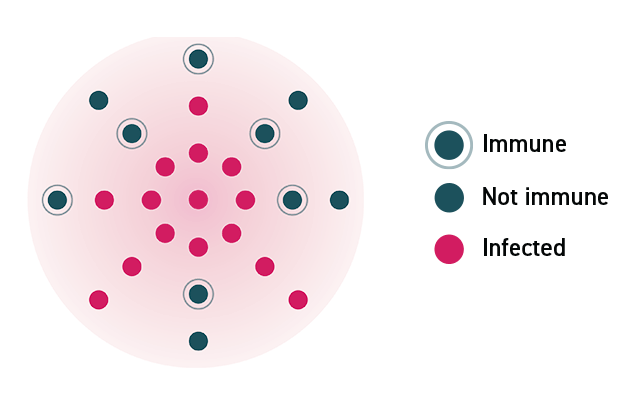
In a community where no one is immune to a virus, a disease can spread rapidly and lead to an outbreak. As individuals acquire immunity, either through infection or a vaccine, the disease spreads more slowly because fewer people can pass it on.
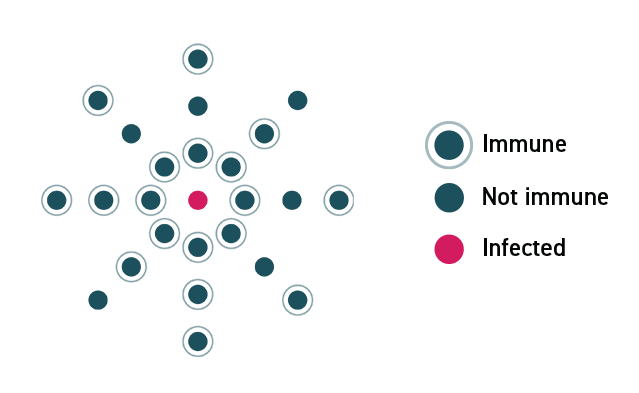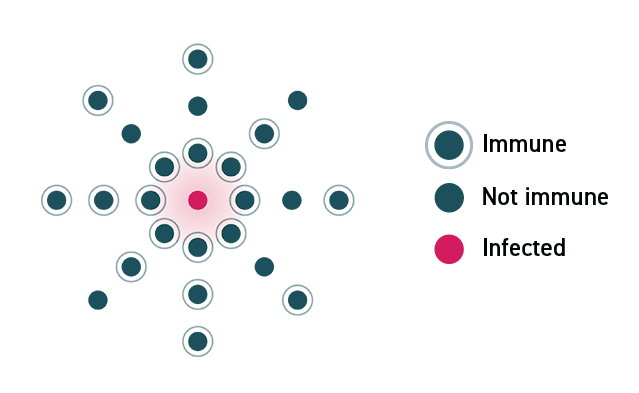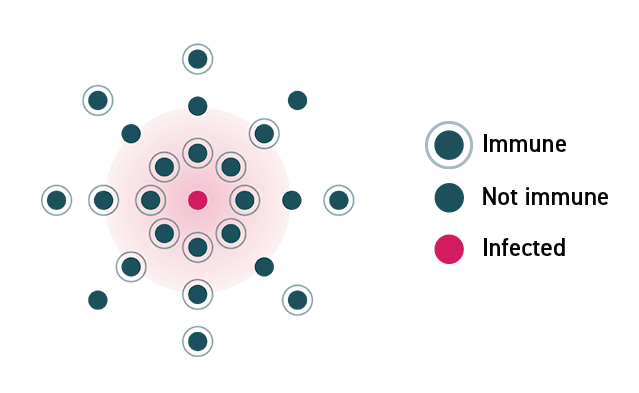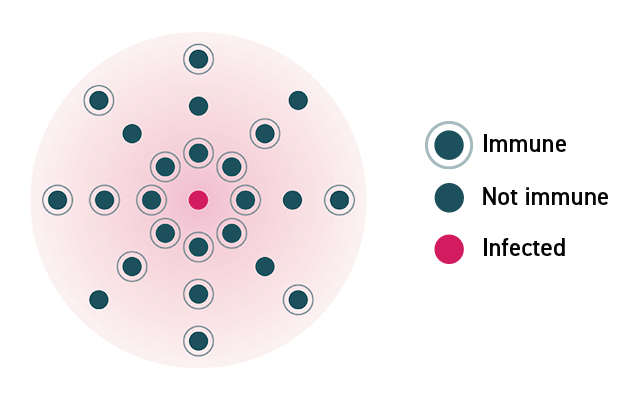
In a community where enough members are vaccinated, the disease will stop spreading because the virus will not be able to find susceptible hosts.
The herd immunity threshold (HIT) varies depending on a variety of epidemiological factors. The primary consideration is the infectiousness of a disease, often referred to as R0; herd immunity helps R0 drop below 1.
“The higher R0 is, you’ll have to have really, really high [levels of active immunity], or it’s still transmissible and the vulnerable population will still get it,” Thompson-Brazill said. For example:
Measles

R0:12-18
93-95%
HIT
Via the Centre for the Mathematical Modelling of Infectious Diseases, London School of Hygiene & Tropical Medicine
Numbers for COVID-19’s R0 have evolved throughout the pandemic, particularly as COVID-19 has mutated into different strains. For example, the highly contagious delta variant was estimated to have an R0 of about 6 to 7, NPR reported in August 2021. That means the delta variant was more than twice as contagious as the original COVID-19 strain, according to the CDC. And the omicron variant has been estimated to be up to three times as infectious as the delta variant.
Although 2020 predictions placed COVID-19’s herd immunity threshold between 60% and 70% vaccination, a March 2021 report in Nature called herd immunity for the novel coronavirus “probably impossible” based on factors including uneven global vaccine distribution, new variants, and changing human behavior.
Natural infection and vaccination could create paths to herd immunity for COVID-19, but there are challenges to both approaches. Natural infection could overwhelm health care systems as millions experience sickness. And reinfection creates additional problems: Those who have contracted COVID-19 can get it again — and it is not clear how long antibodies offer protection after individuals have recovered. It is also unclear how long vaccines offer protection from the virus, which is why the CDC is encouraging eligible individuals to receive booster shots. Vaccine hesitancy could also make achieving herd immunity through vaccination more difficult.
The Role Clinicians Play in Herd Immunity and Vaccination
Zschaebitz and Thompson-Brazill have years of experience in various health care settings— from travel clinics and trauma units to international research. Some of the ways that clinicians increase herd immunity and vaccination include:
- participating in global research to genotype communities and help produce viable vaccines.
- administering vaccines so patients can stay up-to-date on immunization schedules and travel requirements.
- educating patients on the importance of vaccination and the specific information related to different vaccines.
How to Talk to Family and Friends About Vaccines and Herd Immunity
Thompson-Brazill shared her experience speaking with patients who are vaccine-hesitant and said she has learned that one of the roles clinicians play in herd immunity is educating patients about why vaccines are safe and normative for society.
Zschaebitz also shares the importance of herd immunity with patients — often through the retelling of her own experiences genotyping Maasai tribal women for an HPV vaccine.
“We were interested in preventing deaths of cervical cancer because in certain countries women just die,” she said. “Declining a vaccination is sort of a first-world problem because people in other nations would walk for miles to get what we have and what we take advantage of.”
Below are Thompson-Brazill and Zschaebitz’s tips for speaking to vaccine-hesitant friends and family.
Tip #1: Avoid pointed questions that could make someone defensive.
Tip #2: Use storytelling as a way to share your experience.
Tip #3: Refer loved ones to credible, reliable sources.
Tip#4: If you do not know how to respond, recommend an expert who does.
Herd Immunity: FAQ
Is it possible to achieve herd immunity without a vaccine?
Because the herd immunity threshold is so high, achieving herd immunity without a vaccine is unlikely, according to the American Lung Association. The likelihood depends on the disease’s R0, because a lower threshold would be easier to reach naturally. However, the severity of a disease could also mean that many individuals in a community would succumb to a disease before broader immunity is obtained.
Is herd immunity effective against all diseases?
No, not all diseases can be overcome with herd immunity. For example, herd immunity cannot be achieved for Clostridium tetani, the bacteria that causes tetanus. Although infection is avoidable via individual vaccination, the “herd” cannot provide protection. For example, the immunity of others will not prevent an individual from contracting tetanus after stepping on a rusty nail.
Can you still get COVID-19 after being vaccinated?
Breakthrough infections of COVID-19 are still possible for individuals who are vaccinated against COVID-19 because the vaccines are not 100% effective at preventing infection. However, most people who contract COVID-19 are unvaccinated, according to the CDC. Fully vaccinated individuals who later get COVID-19 are less likely to be hospitalized or die from the virus. Protection against the virus also decreases over time and as new variants emerge, which is why booster shots can help to prevent severe disease.
Can you still get the flu after a flu shot?
It is possible to become sick with a strain of influenza that the vaccine was not developed to protect against. However, the CDC says that the flu vaccine will minimize the severity of symptoms among those who do get sick. Other reasons someone could experience flu-like symptoms after getting a flu shot include contracting a different respiratory illness and exposure to the flu virus shortly before vaccination.
Why do I need to get vaccinated for diseases we already have herd immunity for?
Some immune responses weaken over time, which is why booster shots are so important. Additionally, vaccine refusal can lead to waning community immunity. For example, in 2019, measles outbreaks in New York and Oregon threatened the United States’ 20-year measles elimination status, according to a press release from HHS on measles outbreaks in 2019.
Is immunity from a natural infection stronger than immunity from a vaccination?
Yes. Natural immunity, the result of antibody production after natural infection, is often more effective and longer-lasting than acquired immunity via a vaccine. However, acquired immunity is safer. Some cases of natural infection can be accompanied by symptomatic illness and severe outcomes like pneumonia, liver cancer, and even death, according to an article on vaccine safety from the Children’s Hospital of Philadelphia.
Where to Learn More About Herd Immunity and Vaccines
Both Zschaebitz and Thompson-Brazill recommend using nationally-recognized, expert-led sources to learn more about vaccines, like the CDC, FDA, and NIH. Some of the additional resources available include:
- CDC Immunization Schedules: The CDC-recommended vaccination series and timing schedule for children, adolescents, and adults.
- The CDC Yellow Book: A set of travel health guidelines, including country-specific vaccine recommendations and requirements.
- Questions About Vaccines, FDA: The FDA’s collection of information regarding specific vaccines and approvals.
- The Power of Herd Immunity, TED Talk by Romina Libster: Health researcher Romina Libster tells the story of an H1N1 outbreak in her town and the role of herd immunity.
- Vaccines by Disease, HHS: Vaccine-specific answers to questions such as: “Why is this vaccine important?” and “What are the side effects of this vaccine?”
Citation for this content: Nursing@Georgetown, the online MSN program from the Georgetown University School of Nursing




