How Does the Role of Nurse-Midwives Change from State to State?
In the United States, more expectant mothers are utilizing the expertise and care of midwives than ever before — more than 330,000 births were attended by Nurse-Midwives in 2014.1
While this is almost three times the U.S. rate in 1989,2 it remains far lower than many European and Scandinavian countries where midwives lead care in about half of all births.3
“Some people think of midwives in old-fashioned terms, but that’s not true,” said Georgetown University School of Nursing & Health Studies faculty Cindy Farley, PhD, CNM, FACNM. “We are prescribers. We can work with women who have epidurals, and we’re active in expanding options for women.”
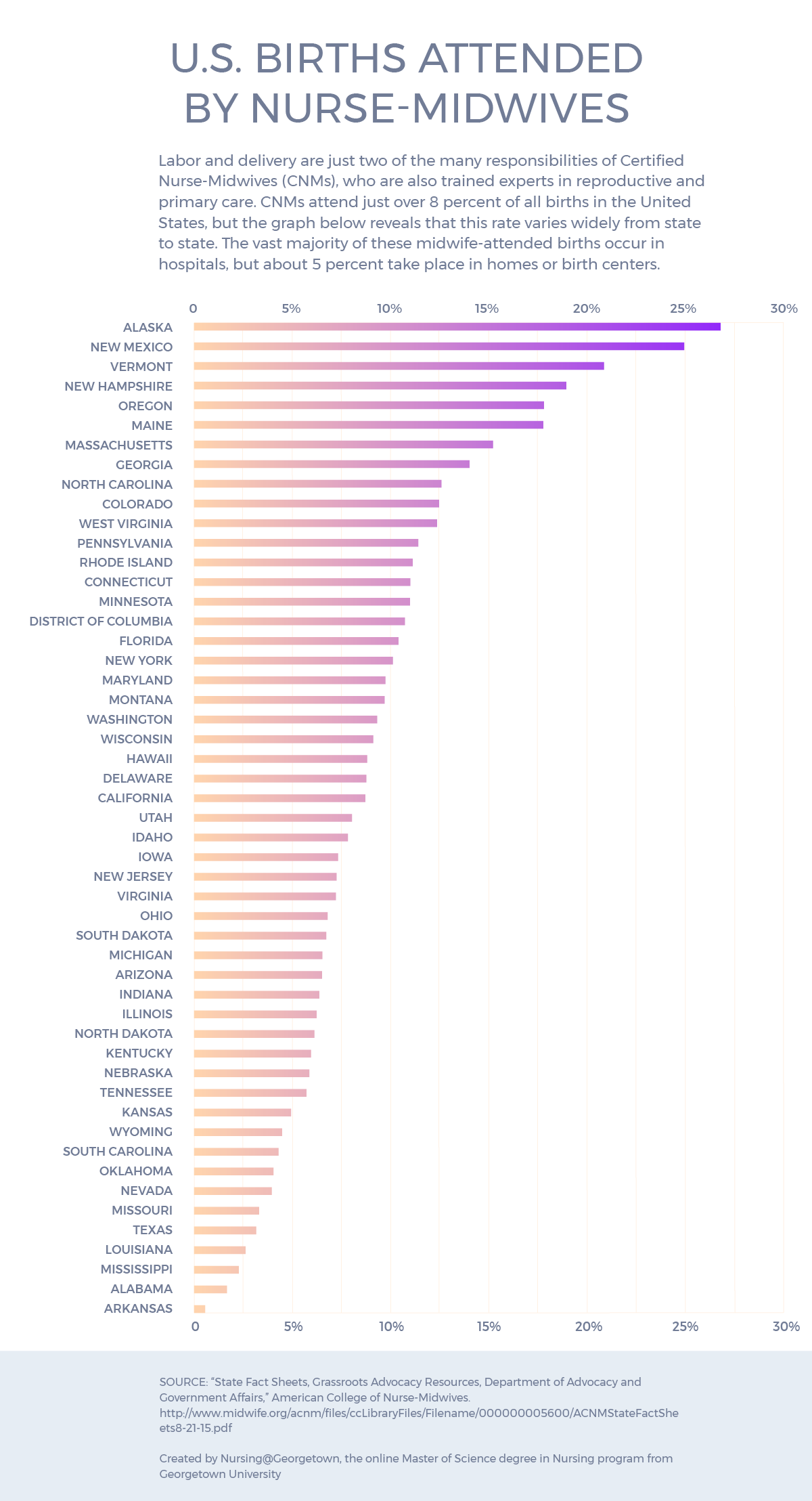
Alaska is the state with the most midwife-attended births, and Arkansas is the state with the fewest such births.
Go to a tabular version of the percent of births attended by midwives, by state.
What can midwives do for patients?
One of many childbirth options in the United States, the midwifery model of care focuses on providing low-intervention births, forming strong relationships, and helping expectant mothers be full participants in their health care.
Not all midwives can legally operate to the full extent of their education and training, as federal and state regulations determine the scope with which Nurse-Midwives practice.
Certified Nurse-Midwives (CNMs) are registered nurses who receive master’s level training in midwifery and who are qualified to attend deliveries in settings ranging from the home to the hospital. Certified Midwives (CMs) also earn a graduate degree but do not have to be a registered nurse prior to entering a program of study. While CNMs are authorized to practice in all 50 states, the CM license is recognized in just five states.
According to the American College of Nurse-Midwives, the midwife cares for babies up to four weeks old and offers care to pregnant women before, when, and after the child is delivered. CNMs are also trained to lead care beyond just labor and delivery. Farley said that Nurse-Midwives work throughout a woman’s life span and can facilitate annual exams, treatments for common infections, and hormone treatments
Every state has a designated practice environment for Certified Nurse-Midwives — independent, collaborative, or supervisory. However, the American College of Nurse-Midwives states that an independent practice authority best enables Nurse-Midwives to use their skills and judgment in helping patients.4
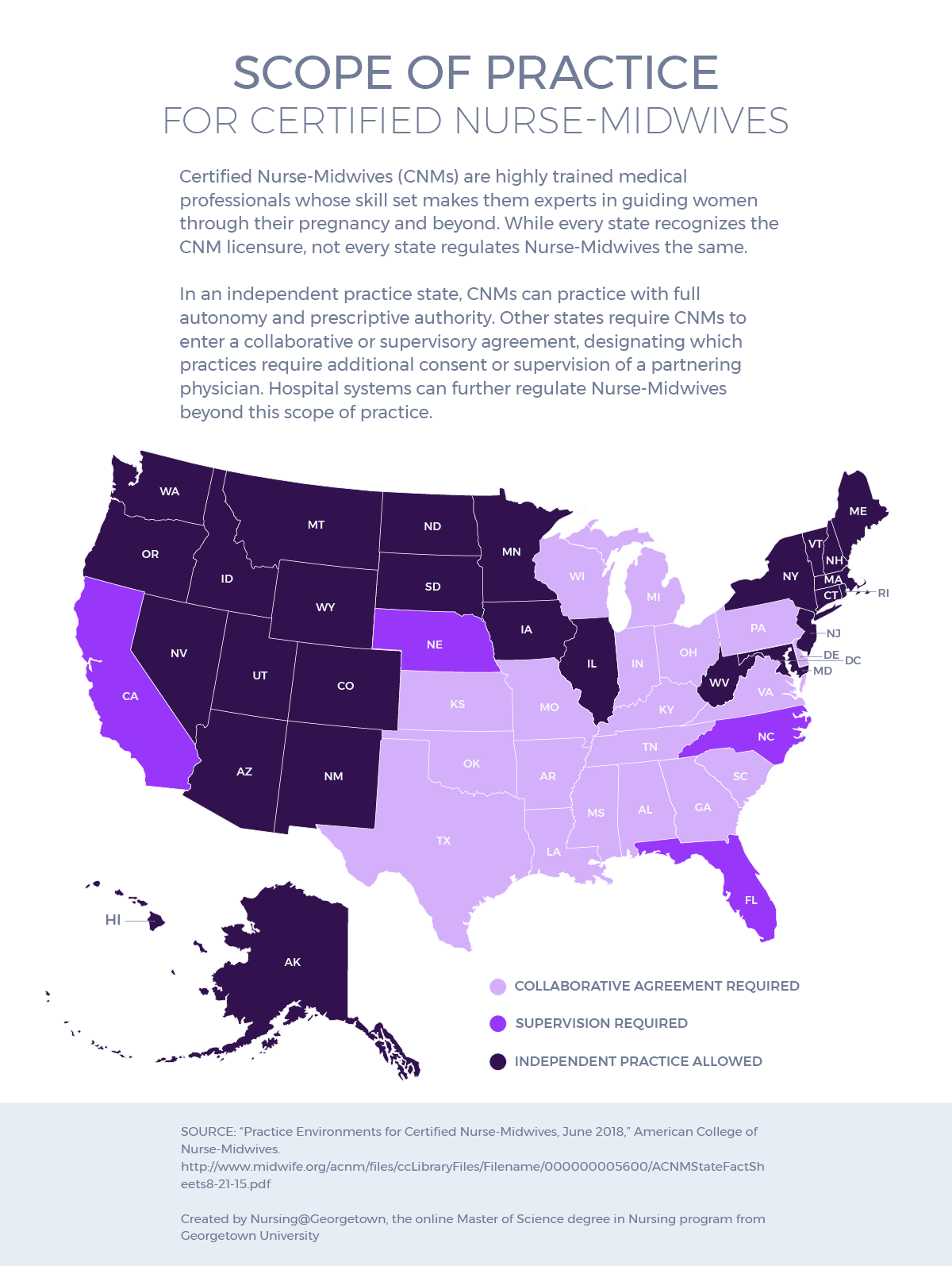
In an independent practice state, CNMs can practice with full autonomy and prescriptive authority. Other states require CNMs to enter a collaborative or supervisory agreement, designating which practices require additional consent or supervision of a partnering physician. Hospital systems can further regulate Nurse-Midwives beyond this scope of practice.
Go to a tabular version of the practice environment, by state.
Why are midwives such an important member of the patient-care team?
Midwives are associated with positive outcomes in part because of their approach, according to Farley. Almost one-third of all births in the United States are cesarean sections,5 twice the World Health Organization’s target rate for cesarean sections.6
“When you just treat women according to their needs and not according to some hospital policy or convenience of staffing, you get better results,” Farley stated.
One study found that when Nurse-Midwives are better integrated into the health care system through regulations, limited restrictions, and increased access to resources, the rate of cesarean sections declines significantly.7
The same study showed a decrease of preterm and low weight births in states that granted midwives a scope of practice that utilizes all their training.
For these reasons, institutions like the National Institute for Care and Excellence, a health advisory body in the United Kingdom, recommend that at least one midwife be present for every birth.8
“We have to keep going back to legislation,” Farley said, “to make sure … we’re at the table for these discussions, are seen as part of the solution, and are allowed to practice to the full extent of our training and expertise.”
The following section contains tabular data from the graphics in this post.
Percent of Births Attended by Midwives, by State
| State | Percent of all births attended by CNMs/CMs, 2013 |
|---|---|
Alaska | 26.8 |
New Mexico | 24.95 |
Vermont | 20.87 |
New Hampshire | 18.95 |
Oregon | 17.81 |
Maine | 17.78 |
Massachusetts | 15.22 |
Georgia | 14.02 |
North Carolina | 12.59 |
Colorado | 12.47 |
West Virginia | 12.37 |
Pennsylvania | 11.41 |
Rhode Island | 11.13 |
Connecticut | 11.01 |
Minnesota | 10.99 |
District of Columbia | 10.73 |
Florida | 10.41 |
New York | 10.12 |
Maryland | 9.74 |
Montana | 9.7 |
Washington | 9.32 |
Wisconsin | 9.12 |
Hawaii | 8.81 |
Delaware | 8.77 |
California | 8.72 |
Utah | 8.04 |
Idaho | 7.83 |
Iowa | 7.33 |
New Jersey | 7.25 |
Virginia | 7.22 |
Ohio | 6.8 |
South Dakota | 6.73 |
Michigan | 6.53 |
Arizona | 6.51 |
Indiana | 6.38 |
Illinois | 6.24 |
North Dakota | 6.13 |
Kentucky | 5.95 |
Nebraska | 5.87 |
Tennessee | 5.72 |
Kansas | 4.94 |
Wyoming | 4.48 |
South Carolina | 4.3 |
Oklahoma | 4.04 |
Nevada | 3.96 |
Missouri | 3.31 |
Texas | 3.16 |
Louisiana | 2.62 |
Mississippi | 2.28 |
Alabama | 1.67 |
Arkansas | 0.56 |
Back to Percent of Births Attended by Midwives graphic.
Practice Environment, by State
| State | Collaborative | Supervisory | Independent Practice State |
|---|---|---|---|
California | 0 | 1 | 0 |
Florida | 0 | 1 | 0 |
Virginia | 0 | 1 | 0 |
South Carolina | 0 | 1 | 0 |
Nebraska | 0 | 1 | 0 |
North Carolina | 0 | 1 | 0 |
Washington | 0 | 0 | 1 |
New Mexico | 0 | 0 | 1 |
Oregon | 0 | 0 | 1 |
New Jersey | 0 | 0 | 1 |
New York | 0 | 0 | 1 |
Rhode Island | 0 | 0 | 1 |
Arizona | 0 | 0 | 1 |
Idaho | 0 | 0 | 1 |
Montana | 0 | 0 | 1 |
Utah | 0 | 0 | 1 |
Minnesota | 0 | 0 | 1 |
New Hampshire | 0 | 0 | 1 |
Vermont | 0 | 0 | 1 |
Wyoming | 0 | 0 | 1 |
Alaska | 0 | 0 | 1 |
Colorado | 0 | 0 | 1 |
Maryland | 0 | 0 | 1 |
Maine | 0 | 0 | 1 |
Massachusetts | 0 | 0 | 1 |
North Dakota | 0 | 0 | 1 |
Nevada | 0 | 0 | 1 |
District of Columbia | 0 | 0 | 1 |
Connecticut | 0 | 0 | 1 |
Iowa | 0 | 0 | 1 |
Hawaii | 0 | 0 | 1 |
Texas | 1 | 0 | 0 |
Wisconsin | 1 | 0 | 0 |
Delaware | 1 | 0 | 0 |
Tennessee | 1 | 0 | 0 |
Missouri | 1 | 0 | 0 |
Indiana | 1 | 0 | 0 |
Michigan | 1 | 0 | 0 |
Arkansas | 1 | 0 | 0 |
West Virginia | 1 | 0 | 0 |
Georgia | 1 | 0 | 0 |
Louisiana | 1 | 0 | 0 |
Pennsylvania | 1 | 0 | 0 |
Kentucky | 1 | 0 | 0 |
Illinois | 1 | 0 | 0 |
Oklahoma | 1 | 0 | 0 |
Mississippi | 1 | 0 | 0 |
Kansas | 1 | 0 | 0 |
Ohio | 1 | 0 | 0 |
South Dakota | 1 | 0 | 0 |
Alabama | 1 | 0 | 0 |
Back to Practice Environment graphic.
Sources
- “CNM/CM-attended Birth Statistics in the United States (PDF, 72 KB),” American College of Nurse-Midwives, March 2016. Accessed September 21, 2018.↑
- Declercq, E. “Trends in Midwife-Attended Births in the United States, 1989-2009,” Journal of Midwifery and Women’s Health, 2012. Accessed September 21, 2018.↑
- Martin, N. “Does a Larger Role for Midwives Mean Better Care?” NPR, February 22, 2018. Accessed September 21, 2018.↑
- Position Statement: Independent Midwifery Practice (PDF, 77 KB),” American College of Nurse-Midwives, February 2012. Accessed September 21, 2018.↑
- PosiMartin, J. “National Vital Statistics Reports (PDF, 1 MB),” CDC, January 31, 2018. Accessed September 21, 2018.↑
- “WHO Statement on Cesarean Section Rates (PDF, 279 KB),” World Health Organization, 2015. Accessed September 21, 2018.↑
- Vedam, S. et al. “Mapping Integration of Midwives Across the United States: Impact on Access, Equity, and Outcomes,” PLoS ONE, February 21, 2018. Accessed September 21, 2018. ↑
- Gallagher, J. ““Home births are ‘best for many mothers,’” BBC, December 3, 2014. Accessed September 21, 2018.↑


