Addressing the Unique Physical and Nutritional Needs of Bedside Clinicians
Two careers that aren’t typically compared — nursing and construction work — are now a point of mutual interest after the U.S. Bureau of Labor Statistics1 released numbers revealing that bedside clinicians experience significant musculoskeletal trauma on the job.
In fact, statistics show nurses who manually move patients throughout their shifts are more than twice as likely to get injured2 compared to those who don’t. Nursing assistants in particular suffer an estimated 37,000 injuries every year3. These injuries occur because of the unique movements nurses use with patients as part of personalized treatment plans that encourage mobility and social interaction while reducing the likelihood of pressure ulcers.
Clinician, Heal Thyself
There are several measures health care practitioners can take to minimize their risk of injury to both themselves and patients. Responsible handling techniques and assistive machinery — like ceiling lifts, sit-stand devices, transfer aids, and sling lifts — are a part of safety protocols that reinforce appropriate body mechanics for health care practitioners whenever they are manually repositioning a patient.
Meanwhile, targeted exercises that develop the back, core, arms, shoulders, and leg muscles have the potential to reduce the risk of physical strain with the added benefit of increasing strength and flexibility. In addition to endurance, body awareness is required in hospital settings to avoid commonplace falls and trips when dashing from the medication room to the bedside and back.
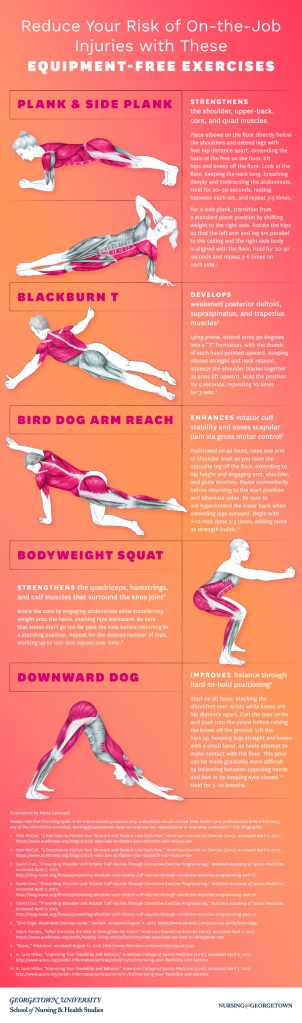
Read the text-only version of this graphic.
The Mechanics of Self-Care
Strengthening the back and core: Research in the American Journal of Nursing shows that in a given year, 39 percent of all nurses4 experience lower back pain. The Journal of Physical Therapy Science found that “core strength training is more effective than typical resistance training for alleviating lower back pain.”5 Core exercises fortify deep trunk muscles like the transversus abdominis and lumbar multifidus, which improve spinal stability, while resistance training tends to focus on shallow muscle groups.6 Care providers who have improper posture while they are documenting patient assessments for hours on end can also benefit from this muscle conditioning.
Developing the arms and shoulders: Research in the Journal of Occupational and Environmental Medicine found that 34 percent of nurses reported “at least one episode of neck/shoulder pain” during a 13-month period.7 Incorrect posture when reaching and pulling at the bedside is the main culprit for those injuries.
Stability in the legs and knees: A nurse walks an average of three miles during an average shift according to research in The Permanente Journal.8 And some walk a lot more depending on patient load and hospital layout. Standing and walking place significant pressure on knees (which bear around 80 percent of total bodyweight), making them more prone to injury, according to the American Council on Exercise.9 Compression socks and rest periods only help so much, so it’s important to practice techniques that support the muscles surrounding the knee to reduce the wear and tear.
Preventing falls with improved balance: According to the Bureau of Labor Statistics, 25 percent of injuries among hospital workers are due to losing footing and falling down.10 That’s where improved balance comes in, via multicomponent exercises that simultaneously increase reaction time and improve coordination.
Direct patient management isn’t the only way caregivers experience workplace injury. Even seemingly benign actions like electronic charting can lead to accumulated strain over time if done with poor posture. A few ergonomic adjustments are beneficial to reduce this risk: The Occupational Safety and Health Administration recommends maintaining a neutral position while typing.11 Hands, wrists, and forearms should be aligned; they should be “parallel to the floor,” and the head should be positioned directly above the torso. Sitting this way helps ease overexertion on bones, muscles, and tendons.12
When not documenting at a computer, clinicians are likely darting from room to room to assess patients when making their rounds. The American Academy of Podiatric Sports Medicine13 advises replacing shoes every 300 to 500 miles to protect the feet from stress and strain. To monitor that accrued mileage, a savvy practitioner can use a pedometer, activity tracker, or cell phone app.
Food as Fuel
Nutrition is another component to workplace health, especially to maintain consistent levels of energy throughout a 12- to 14-hour shift and to prevent accidents related to lightheadedness, nausea, or dips in blood sugar.
Ready-made snacks are a useful source of energy that can be eaten between breaks, especially if they can be safely tucked into a scrubs pocket. Traditional go-to foods for shift clinicians have long included granola bars, dried nuts, and produce like bananas, grapes, cherry tomatoes, and baby carrots. The Academy of Nutrition and Dietetics recommends also consuming a combination of protein and fiber, which promotes satiety.14 Protein blocks mu-opioid receptors in the gut15 to suppress appetite, and fiber delays gastric emptying by creating a viscous solution16 in the digestive tract. Here are three energy-supplying snacks to try:
Apple and Almond Energy Balls
Ingredients:
2 cups rolled oats
1 sliced apple
1 cup almond butter
2 tablespoons chia seeds
2 teaspoons cinnamon
In a food processor, combine all ingredients. Spoon the mixture into rolled balls and refrigerate for 30 minutes until firm. The result will be a portable gluten-free snack that can be stored in the employee fridge and nibbled a serving at a time to maintain energy.
Servings: 25
Grab-and-Go Chia Pack
Ingredients:
¼ cup chia seeds
1 cup almond or coconut milk
1 tablespoon of honey or maple syrup
In a portable container, soak the chia seeds and milk, refrigerating for four hours. Top with honey or syrup and store in the refrigerator until the next break to curtail hunger pangs.
Servings: 2 packs
Roasted Chickpeas
Ingredients:
2 15-ounce cans of chickpeas
2 tablespoons olive oil
½ teaspoon salt
Optional: 2 to 4 teaspoons of cumin, paprika, chili powder, or rosemary
Preheat the oven to 400 degrees before draining and rinsing chickpeas, drying them with a clean towel. In a bowl, combine chickpeas with olive oil and salt, and spread on a baking sheet to oven roast for 20 to 30 minutes. Chickpeas are toasted when they feel crispy on the outside. Sprinkle with the desired amount of optional spice, and sample this savory snack for a quick bite between patient assessments.
Servings: 2 cups
Many people choose a career in direct patient care to make a positive change in the lives of underserved, impaired, vulnerable, and still-recovering populations. Bedside clinicians in particular are trained in hands-on patient management. They collaborate with family members and other treatment providers to craft therapy plans, minimize pain levels, and reduce exposure to infection while advocating for patients in order to improve their outcomes and lower hospital readmission rates.
However, being responsible for the healing of others shouldn’t mean overlooking the care of the caregivers. Pre-emptive safeguards can be taken to fortify frequently used muscles to stabilize and protect against musculoskeletal injuries. Meanwhile, maintaining an adequate eating schedule that takes into consideration the nutritional demands of bedside clinicians ensures providers have the energy to take care of their patients as well as themselves.
Please note that this blog post is for informational purposes only. Individuals should consult their health care professionals before following any of the information provided. Nursing@Georgetown does not endorse any organizations or web sites contained in this blog post.
Citation for this content: Nursing@Georgetown’s Online FNP Program
Sources
- “Economic News Release: Nonfatal Occupational Injuries and Illnesses Requiring Days Away from Work,” United States Department of Labor Bureau of Labor Statistics (2016), accessed April 7, 2017, https://www.bls.gov/news.release/osh2.t03.htm↑
- “Safe Patient Handling and Movement: Guidance for Health Care Workers,” American Physical Therapy Association Learning Center (2011), accessed April 7, 2017, http://learningcenter.apta.org/student/MyCourse.aspx?id=ba540aab-937f-485e-a6ce-48b7fbcb3d3f&programid=dcca7f06-4cd9-4530-b9d3-4ef7d2717b5d↑
- “Economic News Release: Nonfatal Occupational Injuries and Illnesses Requiring Days Away from Work,” United States Department of Labor Bureau of Labor Statistics (2016), accessed April 7, 2017, https://www.bls.gov/news.release/osh2.t03.htm↑
- Susan A. Letvak, Christopher J. Ruhm, and Sat N. Gupta, “Nurses’ Presenteeism and Its Effects on Self-Reported Quality of Care and Costs,” American Journal of Nursing 112, no. 2 (2012), accessed April 7, 2017, http://journals.lww.com/ajnonline/Fulltext/2012/02000/Original_Research___Nurses__Presenteeism_and_Its.21.aspx↑
- Wen-Dien Chang, Hung-Yu Lin, and Ping-Tung Lai, “Core Strength Training for Patients with Chronic Low Back Pain,” Journal of Physical Therapy Science 27, no. 3 (2015), accessed April 7, 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4395677/↑
- Wen-Dien Chang, Hung-Yu Lin, and Ping-Tung Lai, “Core Strength Training for Patients with Chronic Low Back Pain,” Journal of Physical Therapy Science 27, no. 3 (2015), accessed April 7, 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4395677/↑
- J. Smedley, H. Inskip, F. Trevelyan, P. Buckle, C. Cooper, and D. Coggon, “Risk Factors for Incident Neck and Shoulder Pain in Hospital Nurses,” Occupational & Environmental Medicine 60, no. 11 (2003), accessed April 7, 2017, https://www.ncbi.nlm.nih.gov/pubmed/14573717↑
- Ann Hendrich, Marilyn P. Chow, Boguslaw A. Skierczynski, and Zhenqiang Lu, “A 36-Hospital Time and Motion Study: How Do Medical-Surgical Nurses Spend Their Time?,” The Permanente Journal 12, no. 3, (2008), accessed April 7, 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3037121/↑
- Adam Bordes, “What Exercises Are Best to Strengthen My Knee?,” American Council on Exercise (2011), accessed April 7, 2017, https://www.acefitness.org/acefit/healthy-living-article/60/2079/what-exercises-are-best-to-strengthen-my/↑
- Jennifer Bell, “Slip, Trip, and Fall Prevention for Healthcare Workers,” Department of Health and Human Services, Centers for Disease Control and Prevention (2010), accessed April 7, 2017, https://www.cdc.gov/niosh/docs/2011-123/pdfs/2011-123.pdf↑
- “Computer Workstations eTool: Good Working Positions,” U.S. Department of Labor, Occupational Safety and Health Administration, accessed April 7, 2017, https://www.osha.gov/SLTC/etools/computerworkstations/positions.html↑
- “Computer Workstations eTool: Good Working Positions,” U.S. Department of Labor, Occupational Safety and Health Administration, accessed April 7, 2017, https://www.osha.gov/SLTC/etools/computerworkstations/positions.html↑
- Ayne Furman, “How Do I Know When It Is Time to Replace My Athletic Shoes?,” American Academy of Podiatric Sports Medicine, accessed April 7, 2017, http://www.aapsm.org/replace_shoes.html↑
- Tara Gidus, “Eating to Boost Energy,” Academy of Nutrition and Dietetics (2016), accessed April 7, 2017, http://www.eatright.org/resource/food/nutrition/healthy-eating/eating-to-boost-energy↑
- Celine Duraffourd, Filipe De Vadder, Daisy Goncalves, Fabien Delaere, Armelle Penhoat, et al, “Mu-Opioid Receptors and Dietary Protein Stimulate a Gut-Brain Neural Circuitry Limiting Food Intake,” Cell 150, no. 2, (2012), accessed April 7, 2017, http://www.cell.com/cell/abstract/S0092-8674(12)00760-X?_returnURL=http%3A%2F%2Flinkinghub.elsevier.com%2Fretrieve%2Fpii%2FS009286741200760X%3Fshowall%3Dtrue↑
- Candida J. Rebello, Yi-Fang Chu, William D. Johnson, Corby K. Martin, Hongmei Han, et al, “The Role of Meal Viscosity and Oat B-glucan Characteristics in Human Appetite Control: A Randomized Crossover Trial,” Nutrition Journal 13, no. 49 (2014), accessed April 7, 2017, https://nutritionj.biomedcentral.com/articles/10.1186/1475-2891-13-49↑


